
The Affordable Care Act (ACA) and Medicaid expansion represent a significant opportunity to produce better health and economic stability for children and parents together. A new report titled “The Affordable Care Act: Affording Two-Generation Approaches to Health,” released by Ascend at the Aspen Institute and the National Academy for State Health Policy, offers the first comprehensive look at these benefits.
The report identifies two-generation opportunities within the ACA legislation and highlights how they can have a significant positive impact on the lives of low-income families.
Here are five things you need to know from our recently released report:
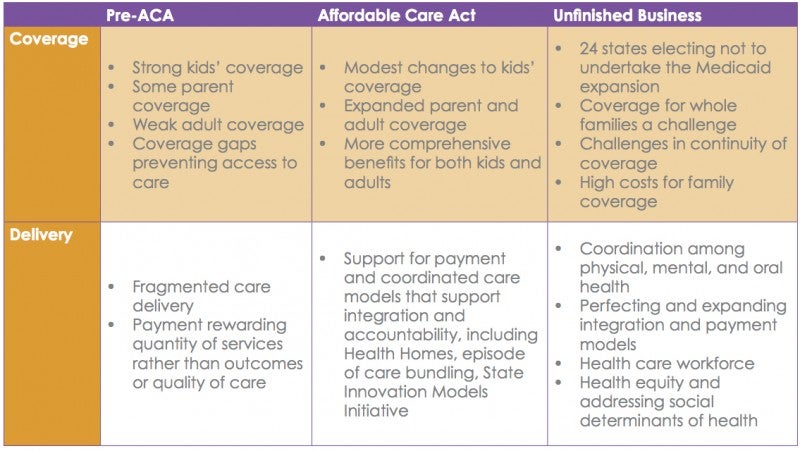
1. The ACA can be transformational in breaking the intergenerational cycle of poverty. Here is how: Good health is a cornerstone of family and child well-being. In fact, family health is tied to income, stability, educational achievement, and strong parental involvement. In 2008, more than 40 percent of non-elderly adults who were uninsured at some point during the year reported being unable to pay for basic necessities, including food, heat, or rent, because of medical debt. Along with federal subsidies for individuals with incomes between 100 and 400 percent of the federal poverty level (FPL), changes brought about by the ACA should lower the uninsured rate for non-elderly adults from 20 percent to 11 percent by 2019.
“The Affordable Care Act is not only the biggest new lever for expanding access to health care, but those of us in communities committed to two-generation solutions see it as a transformative bridge to help break the intergenerational cycle of poverty.”- Anne Mosle, vice president and executive director, Ascend at the Aspen Institute
“The structure of law has a tremendous amount to facilitate access, but there is a lot of advocacy and education that needs to happen.” –Alan Weil, editor-in-chief, Health Affairs
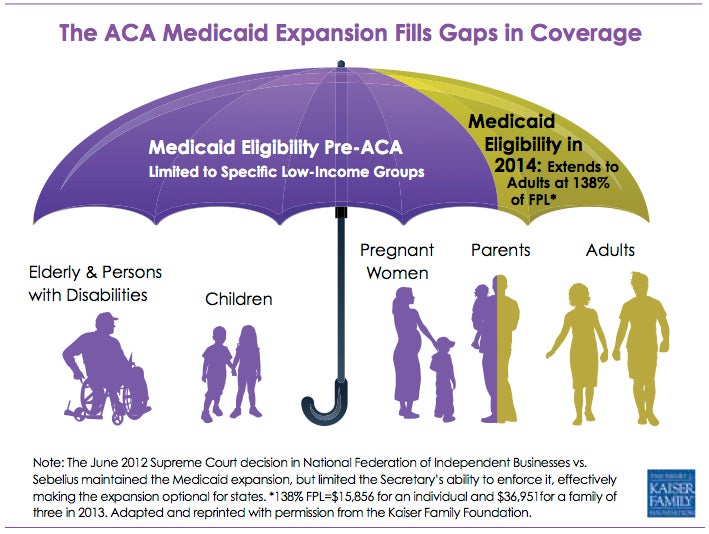
2. Expanding Medicaid coverage and eligibility should continue to be a central focus. As of August 2014, 24 states have declined to expand their Medicaid program. Over half of the 4.9 million parents who were slated to gain coverage through the ACA had no subsidized coverage option in 2014 due to states declining to expand Medicaid. That gap is expected to grow to 6.7 million in 2016. Minorities are disproportionately affected, as many of the states that declined expansion have large shares of uninsured black and Hispanic people. Still, all states are required to make important changes to Medicaid under the ACA, including simplifying eligibility standards and expanding Medicaid for all children up to 138 percent of FPL.
“Medicaid expansion needs to spread, and we need to make sure that the benefits are working for families.” –Liane Wong, Dr. P.H., program officer, the David and Lucile Packard Foundation
3. Health care delivery systems can play a stronger role in promoting intergenerational health and opportunity. New changes under the ACA help to accelerate this potential, including initiatives that incentivize primary care clinicians to deliver comprehensive care and encourage the use of chronic disease prevention programs. The ACA also created the Center for Medicare and Medicaid Innovation, with $10 billion of funding over 10 years, to pilot and scale strategies that move the health care system toward the Triple Aim:
- Improved patient experience of care;
- Improved population health; and
- Reduced per capita health care costs.
“One in 10 moms suffers from maternal depression, with much higher numbers among those in poverty. What is exciting about ACA is how it opens up options to support families. Even the fact that we can do screenings is huge.” –Katie Albright, executive director, San Francisco Child Abuse Prevention Center
4. Advancing the integration of health care systems is essential for improving health outcomes for vulnerable families. The American health care system is still very much oriented toward specialists, who rarely communicate with each other about the patients they have in common. States are pioneering new models of how health care systems can improve integration across physical, mental, and oral health providers, including:
- Coordinated care models through patient-centered medical homes (PCMH): This model has been shown to reduce racial and ethnic disparities in care quality and patient satisfaction.
- Accountable care organizations: ACOs encourage teams of primary care and specialty doctors to accept a fixed payment for a group of people and work together to assure high-quality care. Some states are already testing these models with early successes, such as Rhode Island, Iowa, and Oregon. ACOs in Oregon saw a 30 percent decrease in hospitalizations for heart diseases in the first nine months of 2013.
- Health care workforce development: Scaling new models of care delivery will require educating physicians, nurses, and community health workers. Workforce shortages of health care professionals are acute in rural and inner-city areas, and much work needs to be done to prepare the workforce to meet the needs of a newly insured, aging, and increasingly ethnically diverse population.
“We have to push for innovation but recognize the importance of evidence.” -Dr. Julian Harris, associate director for health, Office of Management and Budget, Executive Office of the President
5. States lead the way in how to combine health and human services to address the needs of whole families. The largest barriers to health for vulnerable families are often unstable living conditions and unmet basic economic needs. Several states, including Vermont, are forming interdisciplinary community health teams that coordinate social workers, public health specialists, and other professionals to provide care and in-home support to families through Medicaid. Another growing trend, “hotspotting,” focuses on the highest-cost and highest-need patients, viewing patients and their needs in the context of their neighborhoods and families.
“The fact is that health insurance is still an individual product… we’ve got to be serious about a family perspective on what it takes to ensure success.” -Alan Weil, editor-in-chief, Health Affairs
Lori Broglio Severens is the senior program manager for Ascend at the Aspen Institute.

